By Ignoring Vaping, Mental Health Orgs Abandon Vulnerable Smokers
Recently, the Royal Australian and New Zealand College of Psychiatrists (RANZCP) came out in favor of the use of vaping products for people who have a psychiatric diagnosis. The organization released a statement saying, “The RANZCP acknowledges that e-cigarettes and vaporisers provide a less harmful way to deliver nicotine to people who smoke, thereby minimising the harm associated with smoking tobacco and reducing some of the health disparities experienced by people living with mental illness.”
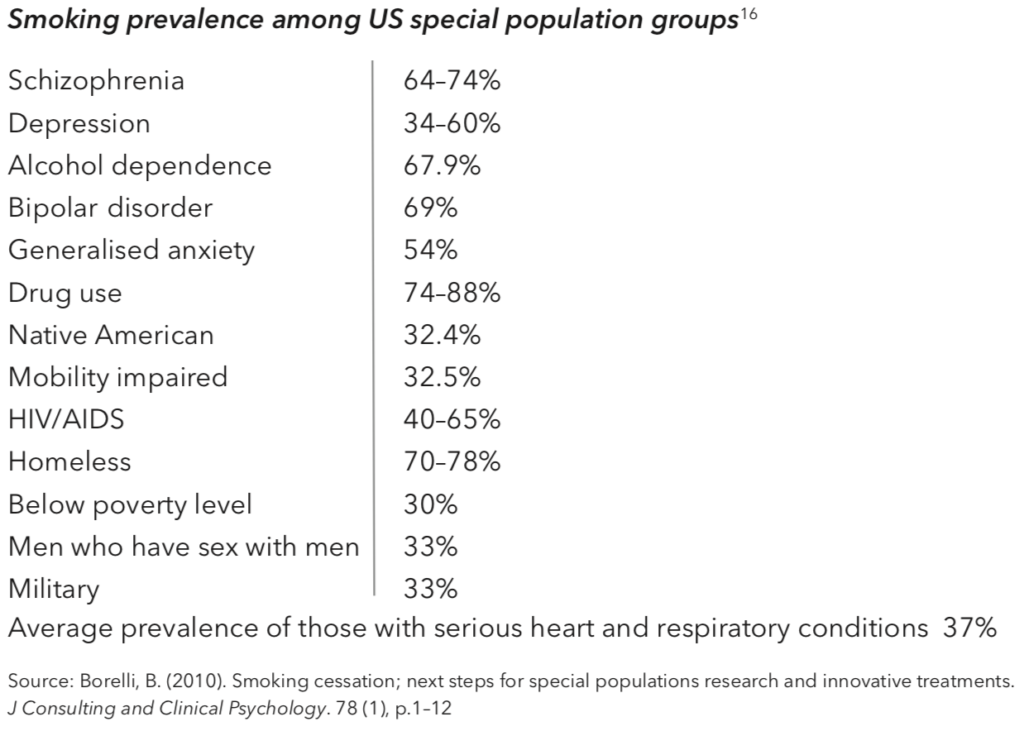
Professional organizations like RANZCP coming out in favor of tobacco harm reduction really matters, because people with psychiatric diagnoses suffer disproportionately from the harms of tobacco smoking. In Australia 70 percent of people with schizophrenia and 61 percent of people with bipolar disorder smoke. But incredibly, Australia has completely banned vaping products. (Vaping advocates there are organizing to end the ban.)
All over the world, people with mental health diagnoses have the highest rates of smoking and:
*Are not only more likely to smoke, but tend to smoke more heavily than the general population
*Have low cessation rates and are less likely to succeed during smoking cessation attempts
*Account for 40 percent of all cigarettes smoked in the US
*Die on average 25 years before the general population
Of the 480,000 people who die in the US from smoking-related diseases each year, it’s estimated that 200,000 had a mental health diagnosis.
Here is some more relevant information:
Given all of these grim statistics, you would think organizations that work with vulnerable populations would be advocating loudly for vaping—which, according to Public Health England, is 95 percentsafer than smoking cigarettes. Millions of people have quit smoking with the help of vaping products.
US Mental Health Organizations’ Abdication of Responsibility
Unfortunately, leading mental health organizations in the US have failed to take a position on vaping.
The Substance Abuse and Mental Health Services Administration (SAMSHA) website provides a wealth of information about the consequences of smoking for people with mental health problems. But their “Smoking Cessation for Individuals with Serious Mental Illness” program doesn’t advocate the use of vaping products. Instead, SAMSHA argues wrongly that “Individuals with serious mental illness do not need to smoke to self-medicate.” Actually, reality shows that they already are self-medicating for the positive effects of nicotine—which has been shown to ameliorate the symptoms of depression and anxiety, and the side effects of psychotropic medications.
The National Alliance on Mental Illness (NAMI) Public Policy Platform states that effective treatment and support for smokers must include: “The most effective nicotine substitution products for individuals with nicotine dependence, as well as other medical approaches with proven effectiveness…” But the organization stops short of specifically mentioning vaping. Neither does NAMI have an official position on vaping on its website. NAMI did not respond to Filter‘s request for comment.
It’s astonishing and unconscionable, given the epidemic of smoking-related morbidity and mortality among people with mental health diagnoses.
Erin Wallace, the chief communications officer at Mental Health America (MHA), did respond, and told me in an email: “We do not have a formal position on [e-cigarettes/vaping].”
MHA does, however, promote “Quitters Circle”—a tobacco cessation program created by the American Lung Association and Pfizer. The pharmaceutical company makes Chantix, a smoking cessation medication. Chantix has a Black Box warning–the most serious type of health alert–which lists side effects such as aggressiveness, suicidal thoughts, hostility and seizures.
Clearly, Chantix poses unique risks for people with a psychiatric diagnosis. Moreover, studies have found that Chantix doesn’t show any benefit over nicotine patches and lozenges, which have low quit rates. The inconvenient truth for the makers of Chantix and nicotine replacement products is that they have failed vulnerable populations. It’s one of the reasons that smoking rates among people with psychiatric diagnoses have not decreased in decades.
This all adds up to an abdication of responsibility by organizations that publicly state they want to reduce the rate of smoking among vulnerable populations. It’s astonishing and unconscionable, given the epidemic of smoking-related morbidity and mortality among people with mental health diagnoses, that these prominent institutions don’t have positions on vaping.
No doubt the junk science on vaping and fear-mongering related to nicotine dependence has contributed to these groups not advocating for the use of vaping products. But vaping is a game-changer for all smokers. Because e-cigarettes deliver nicotine rapidly and replicate the rituals of smoking, people are able to switch more easily.
One Inspiring Example
In contrast to most other countries, the UK has taken the lead in helping people with mental health problems make the switch from combustible tobacco to vaping.
In 2016, Action on Smoking and Health (ASH) released The Stolen Years, a report on mental health and smoking. Among the report’s recommendations: “Evidence-based information should be available to all those with a mental health condition about a range of alternative nicotine containing products including electronic cigarettes.” The report was endorsed by The Royal College of Psychiatrists and Rethink Mental Illness.
“Vaping is allowed in the grounds, and smoking is not.”
At one mental health hospital in Leicestershire, England that was going smoke-free in 2017, staff implemented a program that offered free e-cigarettes to all patients who smoked.
Louise Ross, the program’s Stop Smoking Service Manager, explained: “The patients understood why the wards would become smokefree, but they wanted to use e-cigarettes as a way to manage their nicotine needs. Our policy was written to reflect their views, and every effort has been made to help patients, staff and visitors see this as a positive step forward.”
“Vaping is allowed in the grounds, and smoking is not,” she continued. “This helps to manage nicotine needs while at the same time giving people a chance to try a far less harmful way of using nicotine than by smoking. Nicotine replacement products are also available through the pharmacy on site.”
How many more people have to die before American mental health organizations wake up and endorse the use of vaping products? These organizations must not only take a pro-vaping position, but also make access to vaping products a priority for every smoker with a psychiatric diagnosis.
Helen is the senior editor of Filter. She has written about nicotine, mental health and drug policy for publications including Al Jazeera, AlterNet, Harper’s and The Influence. As an LCSW, she works with drug users in medical and community mental health settings. An expert on tobacco harm reduction, she provides training and consultation on mental health, nicotine use and THR, and in 2016 organized the first Tobacco Harm Reduction Conference in the U.S. Helen is also a documentary filmmaker.
This original post can be found here.






I wanna know vaping is going to effective his mind